If you’ve ever tried to reason with a toddler who has a splinter, you know that “sitting still” isn’t always in their vocabulary. Now, imagine the same scenario, but in a dentist’s chair for a procedure such as a composite resin restoration or a pediatric crown. It’s enough to make any parent’s heart race!
As parents, we want our children to have healthy, beautiful smiles that boost their confidence, but the word “sedation” often brings up a cloud of “what-ifs.” You might be wondering: Is it really necessary for a cosmetic fix? What are the actual risks? Will my child be okay? You’re not alone in these questions. Every year, an estimated 100,000 to 250,000 pediatric dental sedations are performed in the United States. Whether it’s to help a nervous child stay calm or to ensure a complex procedure is done with precision, safety is the number one priority for both you and your dentist.
In this guide, we’re going to look at the complex data, the safety protocols used by American pediatric dentists, and what you need to know to keep your little one safe and smiling.
The “Safety First”
When it comes to your child, “mostly safe” isn’t good enough. You want to know the “why” and the “how.” Research shows that when sedation is administered by a trained pediatric specialist in accordance with the American Academy of Pediatric Dentistry (AAPD) and American Academy of Pediatrics (AAP) guidelines, the success rate is remarkably high.
Key Safety Statistics:
- Success Rates: One study on deep sedation in pediatric dentistry reported a 99.6% success rate, with complications being rare and immediately manageable by the dental team.
- Adverse Events: While major complications are rare, minor “adverse events” (like nausea or agitation) can occur. Data suggests that in outpatient settings, minor events may range from 8% to 47.5%, depending on the depth of sedation and the child’s temperament.
- The Difference in Expertise: Pediatric dentists undergo 2–3 years of additional specialized training beyond dental school, focusing specifically on child psychology, growth, and—crucially—sedation pharmacology.
Why Use Sedation for Cosmetic Procedures?
You might wonder if sedation is “overkill” for something like a dental bonding or a white crown. However, in pediatric dentistry, “cosmetic” often overlaps with “functional.” If a child has significant decay or a fractured front tooth, the cosmetic dentistry procedure requires them to be perfectly still for an extended period to ensure the materials bond correctly and look natural.
Common Levels of Sedation:
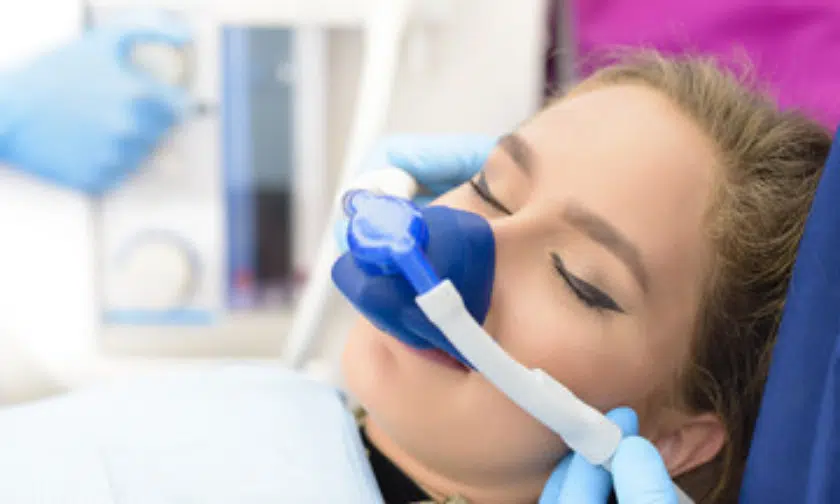
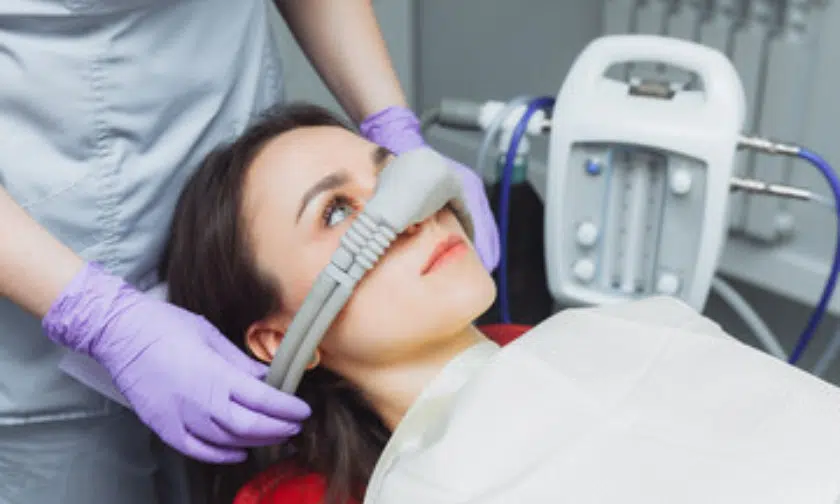
- Nitrous Oxide (Laughing Gas): The “Gold Standard” for mild anxiety. It’s inhaled through a mask and wears off within minutes.
- Oral Conscious Sedation: A liquid or pill that makes the child drowsy but still able to respond to touch or speech.
- IV Sedation: A deeper level of relaxation administered via the bloodstream, usually reserved for more extensive work or children with extreme dental phobias.
The Safety Checklist: How Professionals Protect Your Child
The American Academy of Pediatric Dentistry (AAPD) and the American Academy of Pediatrics (AAP) have established strict guidelines for any sedation or anesthesia in children.
Pre-Sedation Evaluation
Before a single drop of sedative is used, a thorough health history is required. Factors like obesity, obstructive sleep apnea, or enlarged tonsils can increase respiratory risks. In fact, children with developmental disabilities have been shown to have a threefold increased incidence of oxygen desaturation (drops in blood oxygen) during sedation.
Continuous Monitoring
Safety isn’t a “set it and forget it” process. The dental team must monitor:
- Oxygen Saturation: Using a pulse oximeter.
- Heart Rate and Blood Pressure.
- Ventilation: Ensuring the child is breathing effectively.
The “Rescue” Rule
The AAPD requires that any practitioner administering sedation must be trained to “rescue” a patient from a deeper level of sedation than intended. For example, if your child is under moderate sedation, the dentist must be equipped and trained to handle a transition into deep sedation if it occurs unexpectedly.
What You Can Do as a Parent
While the dentist handles the clinical side, you are the most crucial member of the safety team.
Level of Sedation Matters
Sedation levels range from:
- Minimal Sedation — child is relaxed but awake
- Moderate Sedation — conscious but less aware
- Deep Sedation — child won’t be awakened easily
- General Anesthesia — complete unconsciousness
The more profound the sedation, the more monitoring and qualifications are required.
Setting Makes a Difference
Outpatient office sedation can be safe — if the office is adequately equipped and staffed. But serious incidents, including rare deaths, have occurred when guidelines were not followed.
This is why many offices choose to perform deep sedation or anesthesia in a hospital or surgery center rather than an office setting.
Communication With Your Dentist Is Key
Before sedation, you should have answers to questions like:
- Who will administer and monitor the sedation?
- What training and certifications do they have?
- What emergency equipment and protocols are in place?
- What are the risks specific to my child’s age and health?
A good pediatric dentist welcomes this dialogue.
Are There Reported Tragic Cases?
Yes. Although rare, tragic outcomes have occurred, sometimes involving sedation or anesthesia in pediatric dental settings. In 2025, a 9-year-old girl died following a dental procedure involving anesthesia — a reminder that even routine procedures carry risk, especially when safety standards may not have been fully met.
Incidents like this do not mean sedation is unsafe overall — but they DO highlight the importance of high qualifications and strict adherence to safety protocols.
Weighing the Risks vs. the Benefits
Let’s be honest: the idea of sedation can be scary. But untreated dental disease in children is not harmless either. Untreated decay can lead to:
- Pain
- Abscesses
- Infections that spread
- Long-term dental anxiety
- Difficulty eating or speaking
Sedation dentistry, when used appropriately, can allow children to receive necessary dental care with less trauma. Many parents report that sedation helped their child overcome fear and remember the experience with much less distress.
The key is judicious use, proper monitoring, and trained professionals.
Questions to Ask Your Pediatric Dentist Before Sedation
Here’s a handy checklist to take with you:
- What type of sedation is recommended, and why?
- Will the sedationist be on-site, or will a specialist?
- Are vital signs monitored continuously?
- What emergency protocols are in place?
- Has the staff faced any sedation-related complications?
Conclusion
Is your child safe? Yes—when the proper protocols are followed. Pediatric dental sedation is a vital tool that allows children to receive necessary (and cosmetic) care without the trauma of a frightening experience. By choosing a board-certified pediatric dentist in Puyallup who adheres to the joint AAP/AAPD guidelines and by being an informed, transparent advocate for your child’s health history, you can feel confident in their safety.
A beautiful smile is essential, but a safe journey to that smile is what matters most.
Frequently Asked Questions
- Is sedation essential for my child’s dental procedure?
Not always. Sedation is typically recommended when behavior management alone isn’t sufficient for safe and effective treatment. - Are cosmetic dental procedures riskier than other dental work with sedation?
Risks are tied to sedation, not specifically cosmetic work. The key is the level of sedation and how it’s administered. - Can I stay in the room while my child is sedated?
Policies vary, but parents often are not allowed in the room during moderate or deep sedation to ensure safety and monitoring. - What are the most common side effects after sedation?
Temporary nausea, grogginess, and mild agitation are common; serious events are rare, particularly when monitored professionally. - Should I choose a hospital setting over an office?
If your child needs deep sedation or general anesthesia, many experts recommend a hospital or surgery center due to stricter monitoring and emergency support.